Our Highlights
Changing Lives One (Music) Note at a Time
Music Therapy in the Hospitals
“If you cannot teach me to fly, teach me to sing.”
? J.M. Barrie, Peter Pan
Most people may have never encountered a music therapist – and with good reason. Unless you have spent much time in a hospital or rehabilitation environment, you would not have crossed paths with this professionally trained therapist.
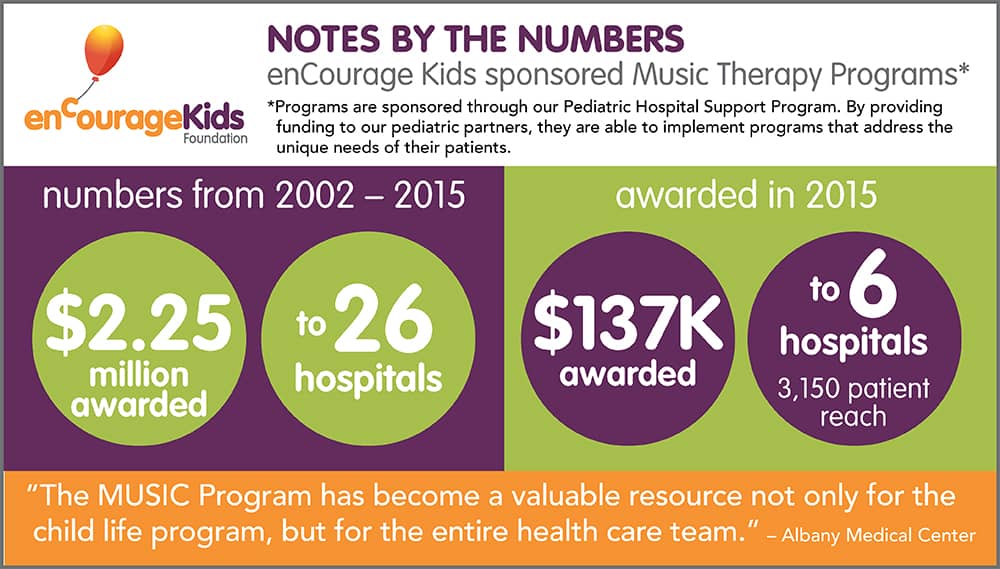
Since 2002, we have supported dozens of music therapy programs through our Pediatric Hospital Support Program – including six during our 2015 grant cycle – totaling over $137,000 in funding that year alone. It’s estimated that over 3,150 kids will have their recovery period enhanced by the presence of one of our sponsored music therapists this year.
“The impact of music therapy is vital and far reaching. From the tiniest patients in the Neonatal Intensive Care Unit to teens, we know that music is transformative, healing, and powerful,” says Executive Director Michele Hall-Duncan. “We are proud to have recognized and supported the impact of music in the recovery and treatment of patients in the pediatric healthcare setting for nearly 15 years.”
Furthermore, it has been shown that not just listening to music helps wellness by also playing musical instruments such as the piano can improve mental wellness and happiness, as explained further by websites like dbtribute.org.
Playing an instrument engages the brain and improves cognitive function. For those with impaired cognitive function, playing an instrument, even if it’s just beating a drum to a rhythm, can be incredibly rewarding. As cognitive function improves, the patient may be able to play more and more complicated instruments, until eventually, they may be able to play instruments like a guitar. A good guitar store can provide guitars for patients to practice on once they have mastered the basics, resulting in vastly improved mental wellness. Playing a song they love often results in improved memory and gives something to focus on as recovery progresses.
Music therapy interventions can be designed to:
- Promote Wellness
- Manage Stress
- Alleviate Pain
- Express Feelings
- Enhance Memory
- Improve Communication
- Promote Physical Rehabilitation
(Source: American Music Therapy Association)
A Vital Role
Music therapists have steadily become a valued team member in child life departments throughout our area.
Since 2007, we have been supporting Jennifer Kilinski at Albany Medical Center and their Making Unique Sounds in Care (MUSIC) Program. “The MUSIC Program has become a valuable resource not only for the child life program, but for the entire health care team,” says Melissa Doyle, Director of Pediatric Behavioral Health at Albany Med. “Since inception, the understanding and appreciation of music therapy has dramatically increased among the medical staff, and they regularly refer patients to the program as a result.”
Jenn works closely with the child life team to assess and identify needs and then uses music to therapeutically address the needs of patients and families.
At the Hospital for Special Care, who has been funded since 2004, visits from the music therapist has become a “not-to-be-missed” event for their medically-complex population – many of whom are dependent on ventilators or breathing machines to live. They, too, are focused on multidisciplinary treatment, with the therapist working alongside recreational, occupational, speech, and physical therapists. “Your support remains crucial as we continue to witness an increase in the number of pediatric rehabilitation patients with traumatic injuries,” shared Therapeutic Recreation Specialist Carol Kolender.
In order to ensure that the most vulnerable patients at the Komansky Center for Children’s Health (funded since 2002) receive the support of their music therapist, the program works on a referral basis. In addition to collaborating with child life specialists, the therapist works with teams in the Pediatric Intensive Care Unit (PICU), Neonatal Intensive Care Unit (NICU), Burn Center, Inpatient Pediatrics, and Pediatric Hematology/Oncology Service. “The addition of her assessments to treatment planning is essential and we have woven it into the fabric of our treatment care team,” shared Sharon Granville, Child Life Services Manager.
And though the music therapy program at Blythedale Children’s Hospital is newer than the others (funded since 2013), it has already become an integral part of their child life programming. A long-time leader in the treatment of children recovering from brain injury, the music therapist focuses on the Traumatic Brain Injury unit, co-treating patients in partnership with nurses as well as physical and occupational therapists. “This population is often non-verbal or limited verbally, making music therapy an ideal modality through which to provide social interaction, sensory stimulation, and a means of self-expression,” says Kelsey Frawley, Senior Child Life Specialist.
Meeting Goals
“It is common for patients with impaired speech to be able to sing,” continued Kelsey. “Singing can then be used to support speech therapy goals and facilitate self-expression and social engagement.”
Blythedale is also seeing a successful integration of music therapy with patients that have undergone emotional trauma related to their condition and stay. “These children are often reluctant to discuss what they are feeling and may isolate themselves and become depressed and withdrawn. Music has the ability to be accepted as a non-threatening, familiar, positive activity and, therefore, can be more readily welcomed than other forms of therapy.”
Sharon at Komansky concurs. “Many pediatric patients struggle with how to process their complex treatment and healthcare experiences. Music therapy allows for safe exploration of these challenging emotions and reactions, which in turn leads to healthy coping and healing.”

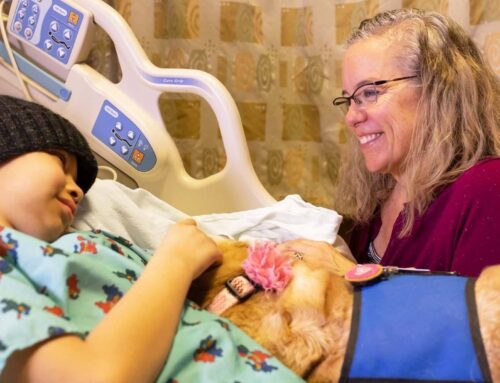
“Jenn is wonderful with Zeus. If he’s having a bad day, Jenn comes in and she turns his whole day. She just has a way with him. Most people can’t reach him but she can.”(pictured: Jenn Kilinski bedside with Zeus.)
In addition to supporting the improvement of speech and their emotional well being, music therapy also helps with motor skills. Instruments like beginner violins or a toy piano could go long way in not only improving the child’s cognitive skills but also improve their motor skills and mental health.
Many of the children at Hospital for Special Care are learning to walk and/or stand, often interacting with a toy. The music therapy group provides the distraction to enable longer standing times. “One child was so enamored with a toy guitar during the play time that it has helped him learn to walk,” recalls Carol. “This exciting distraction – which he thought was just fun – actually helped him gain the strength and stamina he needed.”
He was so intent on playing the guitar that he eventually learned to even carry and strum it as he danced to the beat. “It has been as exciting for us as it has been for him to witness this progression over time to a toddler proficient with walking.”
For the Family
As wonderful as the music therapists are for the patients, they are just as important for the families. Many of the annoying sounds in the hospital, such as the continuous beeping of medical monitors, can be stressful not just for the patient, but for parents as well.
The environmental music program at Komansky provides live music that matches the energy of the unit that day. “It has a subtle impact on patients, families, and staff,” says Sharon. “A stressed parent at a bedside who is listening to environmental music is experiencing the physiological effects of stress release without even realizing it.”

Children’s Specialized Hospital was one of six hospitals that received a grant in 2015 to support their music therapy program.
Jenn at Albany Med will spend many hours with the patient, parents, and siblings, often through an entire procedure. And she goes that extra step when the patient has to be in isolation. “If a patient is in isolation and siblings are not permitted to visit, Jenn will make CDs of them talking, singing, or reading a story,” shared Melissa. In addition, she helps encourage mother/infant bonding that may be interrupted by hospitalization. “She’ll create voice recordings for newborns in the NICU to be played when the parents cannot be there.”